September 23, 2025
Dear Senator Limon,
We present this proposal to outline our legislative priorities for the year 2026, specifically focusing on the introduction of the Communication Support 2.0 Pilot Program. The crisis facing autistic adults in California is urgent: unemployment rates range from 40% to as high as 85%. This leaves 1 million of us underemployed, and 50% Autistic adults are dependent on public benefits. Billions are spent each year on disability programming—over $18.7 billion through DDS, $582.6 million (half-billion) via DOR, and $196.7 billion on Medicaid services. These public dollars flow into bureaucratic processes, restrictive vendor contracts, and programs that fail to deliver meaningful results for the majority. Families are forced to become full-time advocates to pursue even medically-necessary basic communication supports for life.
This is how we see it– we, being the Autistics who are the true stakeholders. The traditional rehabilitation model is designed to “fix” what is broken. A neurodevelopmental difference is not an injury or disease. Adults on the spectrum need policy that prioritizes communication support, not failed attempts at normalization or cure. Investing in true self-expression and autonomy guarantees rising employment rates, reduces Medi-Cal dependency, and restores trust for families. Opportunity, dignity, and meaningful participation for all autistic Californians will mitigate fraud, waste, abuse, and neglect. Across the aisle, our stakeholder plan will succeed.
Duly undersigned:
(1) Henny Kupferstein, PhD, Psychology
Autistic autism researcher
Qualified expert on informed consent for nonspeaking, ASL, and AAC users
(2) Derek Hearthtower
Autistic Guild
(3) Cynthia Velasco, MSHRM, SHRM-CP,
Hermanas Unidas Alumni
Neurodivergent HSP and parent to Neurodivergent children
Advocate for Autistic Children and Adults with a focus on Neurodivergent Latinos
Human Resources Professional
velascocynthia@hotmail.com
(4) Stanley Krippner, PhD
Special education author and teacher
Research Professor, California Institute for Human Science
(5) Jaime Hoerricks, PhD, Education
Autistic gestalt language processor
praeceptor@towcesterabbey.com
Founder and Research Chair – The Praeceptory at Towcester Abbey
Author of No Place for Autism? and Holistic Language Instruction
(4) Martin Friedman, MS Psychology
Neurodivergent, Adjunct Instructor
(5) Anna Aslani MOT, OTR/L
Neurodivergent, Occupational Therapy LEND Fellow
(6) Maria “Des” Valenzuela, MHSW Student
College of the Redwoods
Eureka, CA
Alveraad@gmail.com
(7) Liam Keily, DSP Case Manager
San Francisco, CA
(8) Danielle Owens, DPT
Pelvitone Physical Therapy
San Diego, CA
(9) Aileen Hecht
ASPPIRE of Mid-Michigan, Lansing, MI
(10) Elena E. Tiffany, Autistic Self-Advocate & SD-20 Constituent
NLACRC Consumer Advisory Committee Vice-Chair
SCDD Los Angeles Regional Advisory Committee Member
DDS Lived Experience Advisory Group Member
(11) Alisa Nakano, MA, ASL Teacher, Deaf Advocate
Austin, TX
(12) Katia Zarnegar, MS, CCC
Speech-Language Pathologist, California
Founder, Brentwood Speech Therapy
(13) Sofia Kabir, MS CCC SLP, JD Candidate
CEO and Founder of NeuroSpot Speech OC
(14) Sandra Van Scotter, Autistic, parent of Autistics, Direct Support Professional
Kern Regional Center Self-Determination Program Chairperson
member of the Supported Life Institute Board of Directors
(15) Jennifer Bennett, MA, CRC, CVE
AuDHD, Vocational Evaluator, Advocate, and Consultant, Founder, Pendulum Voc
(16) Timothy Vanscotter, Neurodivergent
timdescendantofscott@gmail.com
(17) Brittany Kalinowski, MS, CCC-SLP
Speech-Language Pathologist
Owner & Director, Monterey Bay Social Language Center
(18) Paul I. McGill, MA, CCC-SLP
Speech-Language Pathologist
Owner & Director, Level Up Speech Pathology
(19) Amy Rowland, MA, CCC-SLP
Speech-Language Pathologist
Owner, Speech Therapy with Amy
(20) Analicia Lucas, MS CCC-SLP
Speech Language Pathologist
Owner of Lake Murray Speech Therapy Inc
License #20898, California
(21) Katherine McKernan-McCracken, SLPD, CCC-SLP
Speech-Language Pathologist
President, North Star Speech and Language Pathology Center, Inc.
(22) India Banks
Speech-Language Pathologist
CEO of Social Butterfly Speech and Language Therapy
(23) Hannah Zimmerman, MA, CCC-SLP
Speech-Language Pathologist
Owner of Just Once Language & Speech Therapy Inc
(24) Henriette W. Langdon, Ed.D., H-CCC-SLP, BCS-CL
Bilingual Speech-Language Pathology
Owner/Partner of Sunflower Therapies
Yes, you have editing permissions. Just click and type. (I will correct formatting errors, no worry)
(25) Christa Sisson, M.C.D., CCC-SLP
Speech-Language Pathologist
Owner of TideSpeak Language & Speech Therapy Inc
(26) Allie Glazer, M.S. CCC-SLP/L
Speech-Language Pathologist
hithere@alliemslp.com
Founder/Owner of alliemslp Speech Therapy Group, Inc.
(27)
(28)
(29)
(30
Henny here: Share please:
or
or
andlinkedin – tag a pro https://lnkd.in/p/gFA22Pkr
or direct link: https://docs.google.com/document/d/16tX8YDYmvffxHz9iJyY4yiWtAxFTVDljPLN_QriG-f4/edit?tab=t.0
Beyond the Rehab Boondoggle: A New Deal for Autistic Adults
2026 Legislative Proposal for California | September 15, 2025
California’s autism systems bilk billions while Autistic adults rot. California has nearly 1-million autistic adults, and at least 17.4% (Use CPM adults (18–64): 18.4% (2023) / 16.5% (2024). Not autism‑specific) are living in abject poverty, and dependent on public benefits (costing nearly $100 billion per year). California is slated to spend over $18.7 billion on everyone who qualifies for DDS in 2026, which includes approximately 4.37% of the state’s estimated 1.2-million autistics. We need lifelong supports, and 85% are unemployed, leaving 928,747 autistic adults unserved. The Vocational Rehabilitation model assumes Autism is something to “fix”, a model that is scientifically and legally invalid. Taxpayers are footing the bill of outdated and harmful programs.

| What it costs | The Waste |
| DDS spends more than $40,000 per-person; 25% consumers are adults | Costs >$7.9-billion for “autism” services for 4.37% of Autistics. |
| DOR spends $250 million/year on 9,150 (approximately 6%) employment outcomes. | Only 1 in 17 DOR consumers are benefitting from DOR. |
| Only between 1% and 2% of autistic adults are unemployable, ($730,000 SSI) | We require lifelong support, regardless of marketable skills. |
The highest cost health and human services programs in California for 2025-26 are led by Medi-Cal (California Medicaid), followed by programs in developmental services, social services, and behavioral health. These programs represent the core of California’s public support for medical care, disability services, and vulnerable populations.
- The Department of Social Services (DSS) receives $56.1 billion in total funds. In-Home Supportive Services (IHSS), a program under DSS, spends $30 Billion a year, double the amount of the Department of Developmental Services (DDS), primarily funded by the California General Fund and federal Medicaid/HCBS waivers.
- DDS only supports 4% of California’s 1-million Autistics from its $18-Billion budget. For the rest of us, the California Department of Rehabilitation (DOR) spends a half-Billion budget on the 1 in 17 chance at successful employment outcomes (9,000 disabled adults removed from SSI).
Rehabilitation is Out of Compliance with Federal Rule
By definition, rehabilitation restores function lost due to illness or injury. For autistic people, their differences are lifelong and not the result of loss, so “rehabilitation” is an inappropriate and discriminatory standard. The Centers for Medicare & Medicaid Services (CMS) dictate that Medi-Cal (California Medicaid) must fund all medically necessary supports for Autistic people, including habilitative services that foster skills never acquired, not just therapies to restore lost abilities. The rehabilitation model does not ensure that medically necessary supports are centered on the actual lifelong needs of I/DD people.
Federal Medi-Cal Law: The HCBS model is also built on providing effective, individualized services in the community at lower cost than institutional or non-individualized care—a goal unmet by rehabilitation programs because they do not produce durable, person-led outcomes.
Beyond Speech Therapy: Supports like communication devices, assistive technology, and individualized mentoring are recognized by federal law as medically necessary for meaningful community participation and least restrictive living, and must be guided by person-centered planning. Communication supports are not “add-ons” contingent upon employment or program compliance.
Mandated by IDEA, ADA, Section 504: Title II entities (State and local governments) and Title III entities (businesses and nonprofit organizations that serve the public) must communicate effectively with people who have communication disabilities. The goal is to ensure that communication with I/DD people is equally effective as communication with nondisabled people.
Rehabilitation makes me feel stupid and lazy.
I am not sick nor injured.
I will be Autistic for the rest of my life
1. California Department of Rehabilitation (DOR)
The California Department of Rehabilitation (DOR) is primarily funded through a combination of federal Vocational Rehabilitation (VR) State Grants, authorized under the Rehabilitation Act of 1973 (as amended by WIOA), and matching state funds. The DOR reported disability categories consist of Blind/Visually Impaired, Cognitive Impairment, Deaf/Hard of Hearing, Intellectual/Developmental Disability, Learning Disability, Not Reported, Physical Disability, Psychiatric Disability, and Traumatic Brain Injury.
The DOR data is not segmented for developmental disabilities. What they call “cognitive” or “developmental” disabilities aligns with the American Psychiatric Association’s DSM multiaxial system from DSM-III (1980). Resultantly, it is impossible to speculate how many autistic consumers are actually benefiting from DOR at all. In 2023, California DOR served about 14,926 I/DD consumers—nearly three times the CDC-based expected autism participant prevalence of 4,968. This demonstrates that state disability programs enroll and support a larger subset of the autistic/DD population than population statistics alone would suggest.
Key Statistics for FY 2025
- Number of consumers served: 154,000
- Successful employment outcomes (closures): 9,150
- 14,926 IDD consumers served (9.79%)
- 1 in 17 successful outcomes = 876 DD/ID individuals
Do we exist just so 483 counselors (p. 63) can have civil service jobs, and California can earn 3x federal match for spending fruitless money?
California’s Department of Rehabilitation (DOR) counts a “successful outcome” based on a consumer achieving a “Measurable Skills Gain” and securing employment that yields a verifiable wage. This is why the main metric for case closure is a reported salary: specifically, a median salary of $4,680.00 earned in the second quarter (three-month period) after exiting the VR program. DOR services are failing to meet the needs of an estimated 1.2 million underserved autistics. DOR spent less than $2,500 per person across all disability groups, for a 17:1 chance at success. (Sources needed)
The End of the Rehabilitation Model
DOR’s work begins with the presumption that all individuals with a disability can benefit from vocational rehabilitation services and should have opportunities to work in jobs integrated within their communities. The wide discretion and implicit bias of potentially-underqualified individual counselors (“bad actor”) often result in non-evidence-based misallocation of services. Inequities across regions or populations fail to serve autistics with demonstrable barriers to competitive employment. In California, 99% of Autistics do not have a permanent disability determination from Social Security, indicating that 1 million of us are potentially employable, unless proven otherwise.
This writer’s DOR counselor made a referral for an assessment designed for identifying unique employment factors, such as strengths, resources, priorities, concerns, abilities, capabilities, interests, and informed choice. The following tests were administered:
- Career Ability Placement Surveys (aptitude tests) include numerical reasoning questions (e.g., “Analyze this graph to determine X”), verbal reasoning questions (e.g., “Based on this passage, what can be inferred about Y?”), and abstract/logical reasoning questions (e.g., “Identify the next shape in this pattern”), as well as personality-based questions about work preferences and social interactions.
- The Wonderlic Personnel Test example questions ask, “How many states are there in the U.S.A?” [A. 20, B. 30, C. 40, D. 50, E. 604] and “There are three times as many elephants compared to giraffes in the safari. If there are a total of 88 elephants and giraffes, how many elephants are there in the safari?”
- Results from the Strong Interest Inventory (SII), a popular vocational interest inventory, compare your responses to those of people successfully employed in different careers to identify your work interests and predict satisfaction. Sample test questions ask you to rate your liking for various job activities (e.g., “Working with heavy machinery”), subjects (e.g., “History”), or leisure pursuits (e.g., “Going to museums”).
- The TABE (Test of Adult Basic Education) is an assessment that measures adult basic skills in Reading, Math, and Language. It is widely used to evaluate an individual’s readiness for further education or training
At the time of assessment, this writer had just completed a Bachelor of Science degree with high honors. The evaluator profiled them as a demographic who: “In this range generally have a tendency to complete 7th grade. With regard to training, participants who score within this range usually do not benefit from formalized training. Representative job titles for this category include: Packer, Material Handler, Custodian & Janitor, Warehouse Worker, Nurse’s Aide and Food Service Worker, among others.”
Under federal DOR law, the DOR counselor’s recommendations can and do supersede “informed choice” when determining which services or supports may be publicly funded. While the policy states that individuals should actively participate and exercise informed choice, the counselor’s professional judgment ultimately governs eligibility, service authorization, and funding decisions. Not a single one of these assessments are clinically validated for existential, humanistic, and transpersonal approximation of human capacity.
Under WIOA and federal rehabilitation law, each state is required to establish and operate a vocational rehabilitation program and report to the federal government that services are being offered to eligible people with disabilities. [WIOA (29 U.S.C. § 720 et seq.); State Plan Requirement (29 U.S.C. § 721(a)(1)); Federal DOR Regulations (34 CFR Part 361) General requirements for state DOR agencies; 34 CFR 361.17 (State agency requirements); 34 CFR 361.40 (Reports; evaluation standards and performance indicators); 34 CFR 361.82 (Reporting requirements).] However, the law does not require the state to provide strong, independent proof that its program is effective at achieving positive employment outcomes. Federal oversight is focused on program existence, minimum service delivery, and reporting, not actual demonstrated effectiveness or impact on participants’ lives.
Faulty methodology correlates with invalidity of approximation of need.
Garbage in, Garbage out.
Bad assessment methods lead to “guesses” about people’s real needs.
2. Medi-Cal Fraud Autism Scheme
Current practice recognizes speech therapy, occupational therapy, and peer mentorship as an effective model for addressing sensorimotor and communication needs, because a communication and movement impairment is part of the autism diagnostic criteria. The ADA and IDEA overlap in their shared goal of ensuring access for individuals with disabilities, particularly through principles like least restrictive communication and environments. Advertised “interventions”, “treatments”, or “cures” cannot be proven as medically necessary because autism as a diagnosis does not immediately entitle an autistic to any publicly-funded support. There is one exception in California, and that is behavior modification interventions modeled after gay conversion therapies, that are now outlawed in 22 states. Survivors have spoken out about these harmful practices.
The Centers for Medicare and Medi-Cal Services (CMS) has not mandated Applied Behavior Analysis (ABA) as a treatment for Autism Spectrum Disorder (ASD) nor endorsed any specific treatment modality, as “autism” by definition is a name of a developmental condition, and not a medical disease. Historically, CMS defines ABA therapy primarily as a crisis intervention. States can interpret what counts as medically necessary. Lawsuits from parents have focused on enforcing access to ABA. California amended its Medi-Cal State Plan in 2014 to explicitly cover ABA under Early and Periodic Screening, Diagnostic and Treatment (EPSDT) for children. Now, ABA coverage applies to all Medi-Cal beneficiaries under 21, regardless of autism diagnosis or Regional Center eligibility, so long as a physician or psychologist recommends it as medically necessary to “correct or ameliorate” a condition. California passed Senate Bill 805, lowering the standards of what a “Qualified autism service provider” is, and further defines ABA as a “treatment” eligible for medicaid reimbursement.
As provider rates are being cut and service caps are implemented, behaviorists are strategizing on how to keep their business booming. Arkansas is enforcing their Child Care Facility Licensing Act now, which requires therapy providers serving five or more unrelated children for more than five hours a day or ten hours a week to be licensed as child care centers rather than as medical providers. Childcare licensing provides mandatory oversight, background checks, and safety standards—measures that would better protect children from harm and ensure public funds are used appropriately. The FBI has continuously found that ABA clinics are used for babysitting, and medical ‘needs’ were fabricated, and AI generated claims overrepresented medical necessity.
In California, licensed behavior analysts and certified behavior analyst assistants are considered “mandated reporters” under California Penal Code §11165.7, which requires them to report suspected abuse of children or dependent adults. Despite holding this legal responsibility, there is no statutory requirement for BCBAs to complete any coursework in psychology or child development as a condition of their certification. So long as parents are not allowed into ABA sessions (they claim it’s their standard of practice), all adults who are enclosed in a space with a vulnerable child should be trained on identifying and reporting suspicions of abuse. It’s a promising sign that Arkansas clinics are shutting down the racket.
Policy change is necessary to correct systemic inequities in autism services. As a federal investigation is in place to recover fraudulent Medi-Cal claims for ABA therapy in the United States, multiple states have initiated a freeze of ABA funding by executive order. A timely departure from aversive therapies that are fraught with controversy, exploitation, and harm will ensure that public funds are used for interventions that respect individual autonomy, support meaningful participation, and comply with federal disability laws. No self-governed Autistic-led advisory committee would recommend public taxpayer dollars to fund the ABA pipeline.
ABA in California is structured in a way that allows a Board Certified Behavior Analyst (BCBA) to open a clinic, hire high school graduates as line staff (Registered Behavior Technicians, or RBTs), and bill Medicaid (Medi-Cal) at high rates—so long as the RBTs are “supervised” by the BCBA, even if the supervision is remote or minimal. Many BCBAs own multiple ABA businesses or franchises and profit by billing Medicaid for vast amounts of “therapy” delivered by an undertrained workforce. This creates a pyramid-like business model in which the majority of billable services are provided by low-wage, entry-level staff while the clinic owner—often a BCBA—maximizes revenue by expanding their franchise under the umbrella of their credentials, rather than the quality of care. This system rewards scale and billable hours over consumer protection, contributing to widespread Medicaid waste and abuse.
II. Communication Support Pilot 2.0
New York’s VR is funded by the State’s Education Department, while VR in California shares coffers with Veterans Affairs. There are 1 million autistics in the state of California, a shared statistic with retired servicemembers. When Communication Support was first introduced to the New York legislature in 2016, Assemblyman Santabaraba asked the State Education to fund these medically necessary supports under the existing Vocational Rehabilitation budget. The American Speech-Language-Hearing Association (ASHA) submitted their letter in support of Bill No. A05141 on behalf of speech therapists. Communication Support, our brainchild, launched a decade ago, and has set a precedent for a new and improved pilot, our 2.0 proposal. The New York 2015 A.5141. Legislation Communication Support service definition:
18 (i) initiating and exiting communication of intent;
19 (ii) topic maintenance;
1 (iii) defusing hostile situations that result from ineffective
2 attempts at independent communication;
3 (iv) preparing, strategizing, and organizing information for written
4 or electronic correspondence; and
5 (v) preparing for upcoming interpersonal communication situations.
An Autism Communication Equity and Support Act (ACES) legislative proposal was submitted to New York’s Governor Hochul in February 2025 to establish universal access to communication support services for autistic individuals in New York. This asked that the $2.1 billion currently misallocated to ABA therapy be redirected to fund Communication Support (our 2.0 pilot) under IDEA, ADA Title II, and Section 504. To date, New York has not suspended Medi-Cal reimbursement mechanisms for ABA, which we the autistics are calling “fake autism therapy.”
The 2015 initiative worked with wild success, and we published the 5-year outcomes in our report for California Assemblywoman Wendy Carrillo, who was interested in Communication Support programs for California. The 5-year outcome report written for California, indicated that successful outcomes peaked during COVID, and we speculate that being offered remote work made job opportunities more accessible to disabled consumers. During the period in which autistic New Yorkers experienced VR employment outcomes (2016–2023), New York’s statewide unemployment rate ranged from about 4.0% (in recent years) up to 7.0% during the COVID-19 pandemic, with pre-pandemic rates typically around 4.1–4.5%. Despite fluctuations in the wider job market, the number of autistic adults achieving successful VR job outcomes remained consistently steady (around 1,000–1,200 per year) since Communication support became a funded service with DOR in 2016.
We have marketable skills
DDS determines a substantial handicap by the scores of the Adaptive Behavior Assessment System (ABAS-3), evaluating communication, self-care, socialization, and community use, to objectively calculate significant functional limitations. Example questions on the ABAS-3 ask about daily skills and adaptive behavior. They include prompts like: “Does this person get dressed without help?” “Does this person use a telephone to make calls on their own?” and “Does this person answer complex questions that require careful thought, such as questions about current events or opinions?”
Supports for employment are not charity but investments in justice and inclusion. Employment confers profound benefits to disabled individuals that cannot be reduced to mere fiscal calculations or the cost to taxpayers for providing necessary supports. The dignity, purpose, autonomy, and social inclusion inherent in employment align with the classic philosophy and the moral codes of all civilized societies—affirming that a human life’s value is never adequately measured by cost-benefit analysis. Cost-benefit approaches to disability supports have been sharply critiqued in legal, philosophical, and disability studies as both logically flawed and morally inadequate, failing to account for non-economic goods and perpetuating discrimination.
We know that Autistic skills and interests such as attention to detail, unique problem-solving, and strong alignment with technical and visual fields, can benefit various professional organizations and truly influence the diversity in the workplace.
- Longitudinal evidence confirms that employment rates for autistic adults increase for those able to access employment experience and individualized supports, regardless of substantial handicap.
- Neither the severity of baseline support needs, nor the degree of autistic traits, can fully predict substantial handicap, which is why we must presume competence unless otherwise proven.
- In fact, workplace experience is the only proven model that correlates with enhancements in adaptive behaviors and social communication skills.
Successful models focus on strength-based initiatives, integrating adults into fields aligned with their passions, supported by interdisciplinary teams. The aim of which is to integrate adults into highly respected and coveted units consistent with their passions, utilizing an integrative team of professional facilitators that included speech and language pathologists, occupational therapists.
How much it costs the state to support me in my daily living may never be used as a measure to deprioritize me in vocational opportunities, under the archaic Order of Selection (OOS) policy. That would go against the moral code of calculating my net burden against my marketable attributes. Sociologists agree that an employed person sees themselves from the lens of what they can do, and psychologists agree that the self-esteem boost one experiences from being in a workplace significantly increases emotional wellbeing. Neurodiversity 2.0 must embrace both opportunities and solutions—creating systems that recognize strengths while actively seeking solutions to address challenges that block access. Generating wealth and proffering financial self-sufficiency for Autistic adults on Medi-Cal must be the logical fiscal priority, reclaiming $100 billion to taxpayers, and with incalculable benefits to society.
Moving Beyond Rehabilitation
Communication Support is the horse for the cart. The idea of “rehabilitating” autistic adults is based on the mistaken belief that autism is a condition to be fixed or cured, rather than a lifelong neurodevelopmental identity. Unlike people recovering from injuries, autistics are born with their differences—they do not need to be “restored” to an imagined norm. Forcing autistic adults into rehabilitation programs that aim to erase natural traits or push unrealistic independence is both a misunderstanding of autism and a violation of dignity.
A neurodevelopmental model honors what autistic people truly need: lifelong support for motor, physical, and communication needs, and not temporary skills assessments that evaluate our deficits. By framing rehabilitation as the primary mandated model for adults, systems perpetuate a harmful idea that disabilities can—and should—be erased with enough training. This can be characterized as a perverse use of public resources, given that it channels funds toward approaches that can cause trauma, limit opportunities, and increase long-term dependency — rather fostering inclusion, communication access, and meaningful employment. Real progress comes from supporting autistic adults as they are, with services that adapt to their real, ongoing needs: communication access, assistive technology, daily living help, and respect for their choices.
Under the current rehabilitation model, the likelihood of IPE development for a DOR-eligible client depends on a caseworker’s perception of the severity of an individual’s disability, to determine whether an IPE would likely benefit the client. Upon eligibility determination, DOR counselors prioritize IPE development for clients whom they deem severely disabled and who will benefit the most from DOR services, to ensure a federal match is guaranteed. Having a master-level education in rehabilitation counseling correlates with highest successful outcomes for DD/ID consumers. At this time, the DOR agency staff capacity is limited by established civil service job classifications (“Voc Rehab Ciunselor”).
Billions for 4% Autistics?
Only those deemed eligible by DDS (the Office for People With Developmental Disabilities) are permitted to enroll in the state’s comprehensive HCBS 1915(c) waiver, which authorizes Medi-Cal funding for a broad array of home and community-based habilitation services. California’s Welfare and Institutions Code 4512(a), part of the Lanterman Act, defines developmental disability for Department of Developmental Services (DDS) eligibility, requiring the onset of the condition before age 22, evidence of indefinite continuation, and substantial handicap to societal functioning. Complete clinical documentation is necessary for eligibility determination, including medical reports, psychological assessments, and adaptive behavior measures.
Specific requirements for documentation include cognitive testing, adaptive assessments, medical reports, and educational records. Functional limitations are evaluated using adaptive behavior measures, with scoring criteria based on standard deviations below the mean. Example questions on the ABAS-3 (Adaptive Behavior Assessment System, Third Edition) ask about daily skills and adaptive behavior. They include prompts like: “Does this person get dressed without help?” “Does this person use a telephone to make calls on their own?” and “Does this person answer complex questions that require careful thought, such as questions about current events or opinions?”.
On standard scoring, a General Adaptive Composite score at least 2 standard deviations below the mean (score of 70 or lower, where mean = 100, SD = 15) objectively documents significant functional limitations. These questions cover areas like communication, self-care, social interaction, home living, health and safety, community use, and work skills. Respondents rate how often the person does each behavior independently, such as never, sometimes, or always, to reflect the individual’s actual abilities in daily life. When DD/ID adults destabilize, mental health clinics must field their crises. OMH takes the heat, because DDS will not service autistics who don’t qualify for services.
Using a highly restrictive and deceptive inclusion criteria, test scores and medical reports of need is considered top secret, and is motivated by the intense protection of the limited budget. Being educable or employable does not require one to tie their shoelaces; Albert Einstein wore slippers instead of laced shoes to save mental energy for his scientific discoveries.
DDS is gatekeeping the federal mandate for autistic Californians. The HCBS Funded program is not open to all Medi-Cal recipients with any disability; it is available only to those who DDS determines meet developmental disability criteria, level of care, residency, and “reasonable indication of need” requirements.
III. Consumer Protection
The Regional Center’s Self-Determination Program (under DDS) mandates consumers like myself to contract with Financial Management Services (FMS) for fiduciary oversight. Unfortunately, these contracts fail to align with standard business practices or licensed financial lender regulations, leaving consumers without mechanisms to enforce fiduciary expectations. This lack of compliance has led to serious consequences, including limited vendor choices, service disruptions, strained relationships with providers due to delayed payments, and other egregious concerns. If an IHSS recipient reports fraud by a provider, the recipient is suspended for 6 months from the program. Again, we adults exist to give jobs to people who are unionized and become eligible for Medi-Cal for having met their minimum work requirement. The care is generic, unskilled, unmonitored, and unregulated.
These issues underscore the urgent need for legislative action to protect vulnerable individuals from systemic predatory practices, and from being used to perpetuate Medicaid fraud. A consumer of publicly-funded programs must have a facilitated and coordinated effort to ensure their rights are mandated into program laws. No employee of a Regional Center, IHSS social worker, DOR counselor, or any affiliated vendor contractors may disparage a DD/ID consumer with impunity. A consumer-reported registry may empower the most marginalized to be heard. We must reasonably consider the case of a conserved adult who is being withheld their SSI and kept in protective supervision by their parents, without an exit strategy toward self determination.
Massachusetts: Nicky’s Law, DPPC Abuser Registry
New Jersey: Central Registry of Offenders
Ohio: DODD Abuser Registry
- Minimum Business Standards and ADA Compliance for Vendors
Amend Lanterman Act and Welfare & Institutions Code §4648(a)(1):
“It is the intent of the Legislature that all recipients of publicly funded social welfare, disability, or developmental services shall be recognized and treated as valued and equal consumers, entitled to dignity, respect, choice, and agency. Utilization of public funds for support or services shall not diminish their standing, rights, or legal protections, nor create or perpetuate stigma, prejudice, or the perception of dependency. All policies, communications, and service practices shall be designed to empower recipients as active, self-determined participants and not as ‘cases’ or passive recipients of aid. Consumers shall retain the full range of legal protections and customer rights available to any member of the public engaging in a civil, transactional, or contractual relationship.”
- Cause of Action and Public Registry
The Lanterman Act has the legal force of a civil statute—conferring enforceable rights and obligations—but does not independently set civil or criminal precedent outside its field. California courts interpret the Act, and those court cases may establish precedent for future Lanterman Act disputes, but the Act itself cannot dictate wider civil or criminal legal doctrine. The Act does not confer new criminal penalties, nor does it control how courts interpret other, unrelated civil or criminal statutes. DD/ID Californians not meeting Lanterman Act eligibility must rely on more general federal and state civil rights laws, which do not guarantee comprehensive, individualized supports or due process—leaving substantial gaps for those consuming public programs but outside regional center eligibility.
Establish a statutory cause of action for consumers and their representatives:
“Any DDS consumer may bring a complaint for ADA noncompliance, unprofessional business practices, or failure to provide effective communication or reasonable accommodation. All substantiated grievances and investigative outcomes shall be recorded in a public registry of vendors, accessible to the public and updated quarterly, for full transparency and consumer protection.”
The Dignity clause: “All publicly-funded (including Medicaid-funded) employees, vendors, and grantees must demonstrate and maintain compliance with the Americans with Disabilities Act (ADA), including accessible communications and public-facing policies. The Department shall set and enforce minimum performance standards based on transparent, universally recognized professional practices.”
Proposed Amendment to California Civil Code (CLRA):
Consumers Legal Remedies Act (CLRA), codified at California Civil Code §§1750–1784, Add Section 1770.1
(a) Right of Action for Public Program Consumers
Notwithstanding any other provision of law, any individual with an intellectual or developmental disability (DD/ID)—or their legally authorized representative—may bring a formal complaint or civil action against any business, service provider, or vendor, including those funded in whole or in part by public funds, for:
- Discrimination;
- Violation of the Americans with Disabilities Act (ADA) or the Unruh Civil Rights Act;
- Failure to provide effective communication or reasonable accommodation;
- Unprofessional, unscrupulous, or unfair business conduct in the provision of goods or services.
(b) Definition of Consumer
For the purposes of this Act, any recipient of services, supports, or goods funded by public programs—regardless of whether the consumer personally transacts the payment or the payment is made on the consumer’s behalf by a public agency or funding source—shall be recognized as a “consumer” with all rights and recourse afforded under the Act.
(c) Remedies
Consumers shall be entitled to all remedies available under the CLRA, as well as injunctive relief, damages, attorneys’ fees, and an order for corrective action or policy change as appropriate.
(d) Registry and Transparency
Substantiated complaints and their resolutions involving public program vendors shall be recorded in a public registry, updated quarterly for consumer awareness and regulatory oversight.
Lanterman Act, Amend Welfare and Institutions Code Section 4731 to add:
“The Department shall be mandated to report to the California Autistic Policy and Equity Commission, and, on at least a quarterly basis, publish and maintain a publicly accessible registry summarizing all substantiated consumer, family, and representative complaints concerning all DDS vendors and grantees. This registry must be updated quarterly to ensure transparency and consumer protection. This section is hereby declared an urgency statute and shall take effect immediately, being necessary for the immediate preservation of public peace, health, or safety within the meaning of Article IV of the California Constitution.”
- Mandatory Vendor Suspension Pending Grievance Resolution
Add to vendor enforcement code and Medicaid waiver oversight:
“Upon the filing of a formal grievance with CAPEC by a DD/ID individual alleging that a vendor, civil servant, or public employee has intentionally or negligently caused them harm, distress, induced a health crisis, failed to comply with the ADA, or committed other misconduct, the subject of the complaint shall be informed of the investigation within 3 calendar days. An investigative outcome in favor of the consumer shall result in immediate suspension of vendor status, and state and federal payments to that vendor will be immediately and indefinitely stayed. This ensures timely deterrence and protects others consumers from potential offenses. The right to file a complaint or seek redress shall not be barred or diminished by the passage of any period of time—regardless of when the alleged incident or conduct occurred.
Proposed Statutory Language: Permanent Registry Record
- a formal record shall be created and maintained in a statewide public registry. This record shall document the complaint, subsequent investigative outcome(s), and the final status, whether substantiated, unsubstantiated, or unfounded.
- The registry and its records shall be maintained in perpetuity, following the model of state child abuse and neglect registry protocols, to ensure accountability, transparency, and prevent future harm to consumers by tracking patterns of conduct among vendors and service providers.”
- CAPEC: California Autistic Policy and Equity Commission (CAPEC) with Legislative Authority
State consumer-led commissions and councils on developmental disabilities are federally funded through the Developmental Disabilities Assistance and Bill of Rights Act of 2000 (DD Act, P.L. 106-402). The DD Act is administered by the Administration for Community Living (ACL) within the U.S. Department of Health and Human Services. About $77–80 million allocated nationally each year, and California typically receives over $3 million for its mandated council and associated policy/oversight activities. Each state receives a federal formula grant to operate a DD Council (or commission/board) for advocacy, consumer protection, and independent oversight. We the autistics need to establish a federally funded, self-governing organization composed of Autistics with specific substantive areas of expertise, and be charged with identifying the most pressing needs of people with developmental disabilities in their state or territory. Funding covers consumer-led engagement, policy work, outreach, legislative recommendations, hearings, and professional training.
Image Description: A group of diverse professionals who utilize assistive technology to amplify their message. Give us the platform and we will figure out how to communicate.
CAPEC: A commission of 24 members shall utilize a $3-million SCDD-compatible operating budget. The Workforce Innovation and Opportunity Act (WIOA) allows federal funds to cover wages or stipends for participants who are placed in paid work experiences or public service opportunities, provided the placement furthers the participant’s Individual Employment Plan and is handled through appropriate program channels. WIOA Title I funds can be used for wage payments “when the work experience is a planned, structured learning experience that takes place in a workplace for a limited period of time,” and stipends are explicitly allowed for participants who further their skills through such service or nontraditional placements.
Section X. Establishment of the California Autistic Policy and Equity Commission (CAPEC)
- Legislative Findings and Intent.
- The Legislature finds that advancing the wellbeing, autonomy, and rights of autistic Californians requires ongoing leadership and input by those most impacted—autistic people themselves.
- The Legislature affirms alignment with the federal “By the People, For the People” initiative and recognizes bipartisan support for equity, self-determination, and civil rights in disability policy.
- It is the intent of the Legislature to establish a permanent, empowered, consumer-stakeholder body to guide policy decisions affecting all developmental and intellectual disability programs under California law.
- Creation and Purpose
- The California Autistic Policy and Equity Commission (CAPEC) is hereby established as an independent, standing commission to the Legislature, the Department of Developmental Services, the Department of Rehabilitation, and all state agencies and bodies administering programs impacting autistic people.
- CAPEC shall have exclusive authority to review, analyze, and issue recommendations on any bill, regulation, or policy that affects the rights or services of autistic Californians before such matters proceed to final vote in the Legislature.
- Membership (24 people)
- No fewer than 70% of CAPEC members shall be autistic Californians, including:
- At least 30% autistic scientists with advanced degrees or equivalent lived experience in autism/disability research or policy.
- At least 20% autistic service professionals and direct advocates.
- At least 20% autistic consumers or direct recipients of DDS, DOR, Medi-Cal HCBS/waivers, or Regional Center services.
- Remaining seats may be filled by family advocates, non-autistic disability professionals, or community allies, provided majority control remains with autistic members.
- CAPEC shall reflect the state’s diversity by race, gender, region, and socioeconomic status, and members must meet strong conflict-of-interest and independence standards as defined in statute.
- No fewer than 70% of CAPEC members shall be autistic Californians, including:
- Powers and Duties
- CAPEC shall:
- Review, hold public hearings, and publish plain-language recommendations for any legislative, regulatory, or policy initiative affecting autistic people.
- Require that no bill or rule affecting autistic rights/services advance beyond any Committee without published CAPEC analysis and public comment.
- Be empowered to call witnesses, subpoena records and internal data, convene forums, conduct research, and require timely agency response to recommendations.
- Ensure full ADA compliance in all operations and public transparency of all materials.
- CAPEC shall:
- By the People, For the People.
- All CAPEC findings and proposals must be written in accessible, plain language and disseminated broadly.
- CAPEC is a permanent, independent, consumer-majority institution at the core of California’s disability policy framework, ensuring that those with lived expertise lead on every decision about their rights and futures.
IV. A Waiver that supports us
California must seek a CMS “benchmark” or demonstration waiver under Section 1115 for people who have communication needs but aren’t institutionally at risk (ICF-level). CMS will expect clear, non-duplicative benefit design, robust evaluation, and a strong rationale for why these services aren’t available through existing programs. The state must make the case for unmet medical need, prevention, and community integration. Autistic-led research should be prioritized, as we are true stakeholders with credible input for CMS application and approval, medical justification, and a new eligibility framework to launch a communications support waiver for non-ICF-level DD adults rejected by DOR.
Although employment is associated with improved quality of life and overall well-being, future research must further investigate what constitutes a ‘good’ workplace or a ‘good’ job in terms of mental health outcomes. Disabled people who are placed in meaningful opportunities consistently have higher competitive employment earnings than those in control or traditional vocational programs, though overall financial gains are modest in relation to public benefits like SSI/SSDI. Autistic people lose their jobs because of communication problems rather than their inability to perform assigned work tasks.
California’s DDS eligibility laws must change. Communication support must be funded when DOR has found autistics to be “unemployable” or “uneducable”, and when IHSS has been unable to help us beyond generic babysitting. We must enact “rehabilitation” as not appropriate for many autistic and DD/ID consumers.
- Clarify DDS Communication Support Eligibility for DOR-Ineligible Individuals
- Amend Welfare & Institutions Code §4512 (Lanterman Act) or the corresponding DDS statute to specify:
- “Individuals with intellectual or developmental disabilities who are found ineligible for employment or education services by the Department of Rehabilitation (DOR) due to a lack of capacity to benefit from rehabilitation—including those with General Adaptive Composite (GAC) scores above 70—shall remain eligible for DDS-funded communication support and habilitation services.”
- Clarify that communication support and habilitation are not medical or rehab “treatment” but essential access services for self-determination. These services must be available without delay, denial, or a “prove medical necessity” gatekeeping approach.
- Amend Welfare & Institutions Code §4512 (Lanterman Act) or the corresponding DDS statute to specify:
- Create a Medi-Cal Communication Support Waiver
- Add a new section to Welfare & Institutions Code or the Health and Safety Code:
- “The Director shall develop and obtain federal approval for a Medi-Cal Home and Community-Based Services Waiver for Communication Support, available to individuals with developmental disabilities—including those above existing GAC or adaptive thresholds—who are unable to sustain competitive employment and have documented, unmet communication needs.”
- Add a new section to Welfare & Institutions Code or the Health and Safety Code:
- Restrict DOR Rehabilitation Obligation for Specific Cases
- Amend California’s Rehabilitation Act or add a clarifying statute:
- “No person with developmental or intellectual disabilities shall be required to prove rehabilitative capacity, employment readiness, or participation in pre-vocational efforts as a prerequisite for accessing habilitation, communication supports, or home- and community-based services through the Department of Developmental Services, when clinical or educational evidence demonstrates such interventions are inappropriate or harmful.”
- “No consumer shall be required to exhaust ‘generic’ resources such as physical therapy (PT), IHSS, or any medical rehabilitation interventions before being authorized for personal assistance, supported living, or communication support. Services supporting self-determination and community integration shall not be treated as secondary to or contingent upon failed medical rehabilitation.”
- Amend California’s Rehabilitation Act or add a clarifying statute:
- Require Integrated Referral and Eligibility Pathway
- Statutory cross-reference between DOR and DDS:
- “If DOR determines an individual is not reasonably expected to benefit from employment or education services, it shall automatically refer that individual for communication supports and ensure that DDS eligibility for such services is not denied solely based on GAC/adaptive functioning scores. A DOR finding of unemployability or lack of educational capacity shall not preclude eligibility for DDS communication, community living, or habilitation supports.”
- Statutory cross-reference between DOR and DDS:
- End the Race to Exhaust “Rehabilitation” Before DDS Access
- Legislative intent declaration or new statutory provision:
- “It is the intent of the Legislature that persons with developmental or intellectual disabilities, who are unable to engage in gainful employment due to disability, are entitled to direct support and communication services—including augmentative and facilitated communication—without the prerequisite of unsuccessful attempts at rehabilitation or DOR services.”
- Legislative intent declaration or new statutory provision:
🎤 This proposal ends the behavioral monopoly on Medi-Cal and publicly funded “autism” services, establishes communication support as a core service in California’s system, and ensures that funding only flows to supports that respect autistic rights and best practices. It expands legal protections beyond those currently enforced by SB 946 and the Lanterman Act, and aligns state law with the strongest federal anti-discrimination mandates. 🎤
[ end of report ]
Appendix Data
In the U.S. in 2024, older adults now outnumber children in almost half of U.S. counties (around 45%), a significant increase from 2020. Autistic poverty can only be calculated by census data of the number of adults reported in the state by year. Autism prevalence for adults is calculated using CDC estimates. SSI recipient data by state is also generating an adult calculation using CDC prevalence rates.
Population demographics
- CA census: 39,538,223 people in the state
- Adult population (18+): Approximately 30,142,124 (76.2% of the total population).
- or 1,276,000 autistic Californians (1.3 million)
- Autistic adults: CDC prevalence, at minimum 971,100 autistic adults
There are an estimated 1 million autistic adults in California equaling that of the 1-million estimated veterans in the State.
Based on the most recent estimates, about 1,569,975 youth (ages 15-17) reside in California. Nationally, 700,000 youths with autism become adults each year (est. 14,000 in CA), and supports and services are needed to improve their long-term success. Our underserved population is nearing 1.3 million in California.
🚨Underserved autistic adults: 1,021,100, including transitioning youth (50,000 autistic).
- Under age 18: 18.6% of children (roughly 1.5 million) live in poverty.
- Age 18 and over: The adult poverty rate (based on aggregate rates for adults and seniors) is approximately 17.4%, which amounts to about 5.5 million adults in poverty. Not autism‑specific
- Given a CDC prevalence, there are approximately 177,419 autistic adults living in poverty in California (based on an adult poverty population of 5.5 million).
CA Department of Rehabilitation (DOR) Budget: $582.6 million (half-billion)
- 2025 DOR consumers: 154,000
- Successful outcomes: 9,150 (6%) 1 in 17
The reporting mandate is very loose, and segmented data simply does not exist. DOR disability categories consist of Blind/Visually Impaired, Cognitive Impairment, Deaf/Hard of Hearing, Intellectual/Developmental Disability, Learning Disability, Not Reported, Physical Disability, Psychiatric Disability, and Traumatic Brain Injury.
- In 2023, there were 14,926 (9.79%) consumers with Intellectual/Developmental Disability.
- CDC prevalence of consumers served: 4,967.74 autistics, at minimum in consumer prevalence.
In 2023, California DOR served about 14,926 IDD consumers—nearly three times the CDC-based expected autism participant prevalence of 4,967.74. This demonstrates that state disability programs enroll and support a larger subset of the autistic/DD population than population statistics alone would suggest.
DOR’s 2025-26 budget allocates about $250 million for case services, serving roughly 100,000 VR consumers annually. This results in an average expenditure of about $2,500 per consumer. Rates and Services Table indicates the most expensive purchase of Service, indicating a range of $17 per hour for “Workplace Readiness Training (WRT)” up to “Customized Employment (CE): Discovery”. These are all unregulated professions with no-bid contract renewals for vendors who do not have to prove effective outcomes.
Deaf and Disabled Telecommunications Program Fund: $3,657,000 is not accounted for, and it is impossible to track how this fund is allocated.This fund provides resources for services and equipment enabling people with disabilities (including those who are Deaf, hard of hearing, have speech or cognitive disabilities, or other disabilities affecting communication) to access telecommunication services. Voice Options is a pilot program of the CPUC’s DDTP and presently administered by the California Department of Rehabilitation. The purpose of the pilot is to provide eligible Californians who are unable to speak, or who have difficulty speaking, with a speech generating device. Communication Support is not a service offered by DOR.
- If CA DOR spends $2500 * 1,021,100 = 2,552,750,000
Legislative Ask: $2.5 Billion Communication Support investment
California Department of Developmental Services (DDS)
- 2025-2026 Budget: $18.7 billion
- Consumers served: 450,000 ($41,5555 per consumer)
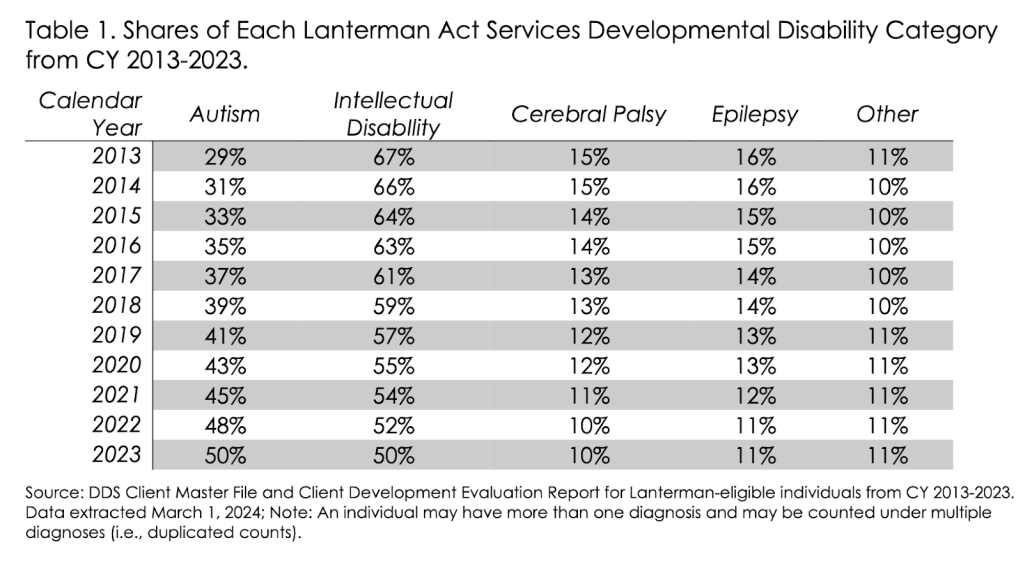
- 51% of all DDS clients have an autism diagnosis (196,756 out of 386,062)
- Approximately $7,910,240,000 for ASD consumers.
- 51% of all DDS clients have an autism diagnosis (196,756 out of 386,062)
- Adults served (25%): 116,217 adults, 42,353 autistic adults (age 18+)
- (4.37% of California autistic adults) ● [→ DDS Autism Report (2025): ASD adults (22+) ≈ 21.5% ≈ 42,300. Source: https://www.dds.ca.gov/wp-content/uploads/2025/05/2025_AutismLegReport_Accessible.pdf%5D
- 1 in 17 of 1,021,100 = 60,065.88 may achieve employment, DOR odds
Only a small fraction is now dedicated to state institutions, with facilities like Porterville receiving $25-million ongoing cuts and most of the funding going toward regional center community-based service. Despite the high costs of institutionalization, these outliers skew the data reports and do not adequate reflect the needs of the majority.
Autism-related DDS expenditures are now in the multi-billion dollar range, with annual totals exceeding $2 billion and covering more than half of all individuals served by the department—making autism services the single largest element within DDS spending. Autistic consumers make up 50% of the service demographic through DDS.
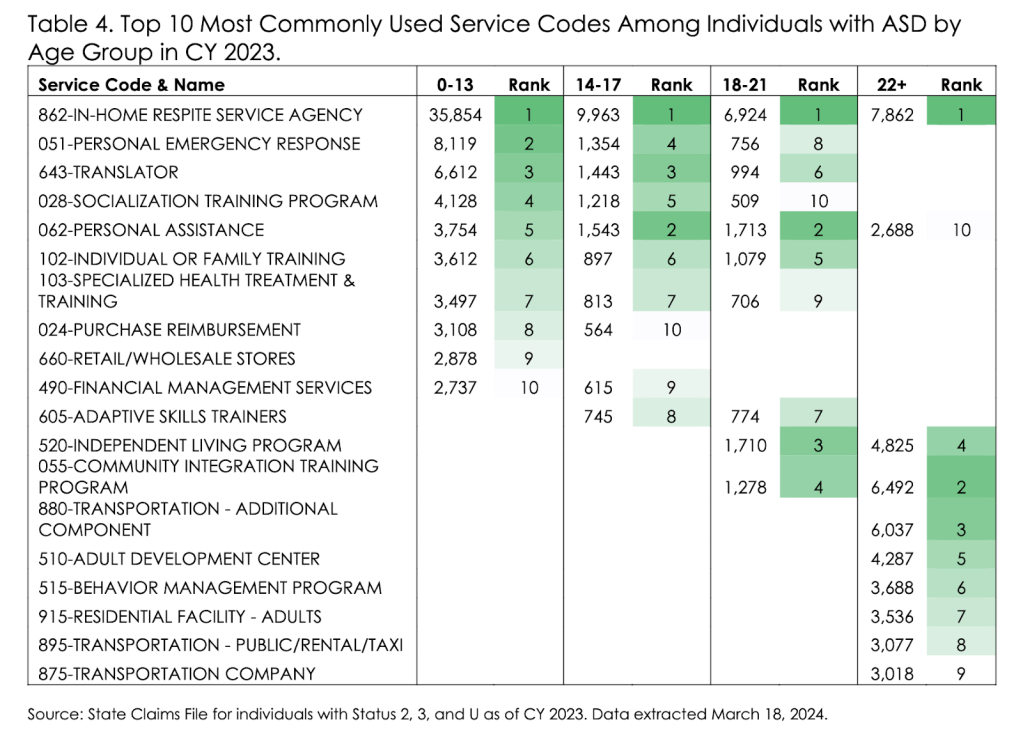
Communication Services not offered for adults. For DDS adults 22 years-of-age and older, residential facilities (service code 915) accounts for the highest expenditure of any service category, accounting for $320,522,64 per consumer, compared to $16,000 cost for a consumer living with their family.
California Medicaid “Medi-Cal”
Roughly 15 million Californians are enrolled in Medi-Cal as of early 2025—making it the largest state Medicaid program in the nation, costing $196.7 billion in total funding for the 2025–26 fiscal year, with $44.9 billion coming from the state’s General Fund.
- Medi-Cal: 14,907,754 enrolled
- Autistics on Medi-Cal: 480,248.55 (47% of autistics)
196,756 Lanterman-eligible individuals with ASD in FY 2023–24 _ Can’t verify the 480,248.55
Annual Report To The Legislature On Autism
- at $8,000 = $3,841,988,400 (nearly $4-billion)
Approximately 15% of enrollees are people with disabilities, costing $20,222 per enrollee. Medicaid spends about 5 times more on a consumer with an autism diagnosis than the overall average Medi-Cal enrollee in California. The average cost for a Medi-Cal enrollee is $8,000 per year, while a Medicaid-covered autistic individual in California costs ~$40,000 per year, an expenditure that is consistent with the national average.
For ABA therapy specifically, Medi-Cal can cover up to $45,000 annually per person for intensive services such as 10+ hours per week of “treatment”.
- If California invests $40,000 on 1,021,100 autistics, not just the 4% served by DDS, that would cost $40,844,000,000 ($40 Billion).
- A $2,500 Communication Support investment = $2,552,750,000 ($2.5 Billion)
Underfunding Medicaid disability services led to a lawsuit (Ligas v. Maram) after thousands of autistics were institutionalized indefinitely due to lack of HCBS. According to the social cost framework of Salkever (2013), reallocating resources from wasteful programs to evidence-based supports raises overall system value without increasing net costs.
In-Home Supportive Services (IHSS) Program
- IHSS 793,000 consumers
- 11% protective supervision = 87,230 ($5.5 Billion)
- 2025-2026 Budget: $29.9 billion
- $37,703.8 cost per person
- Compared to $320,522,64 for DDS adults in facilities
- If 87,230 were to move into facilities, that would cost 27,961,290,017.20 ($27 Billion).
- $37,703.8 cost per person
As of January 2025, the average state IHSS wage in California is approximately $18.66 per hour. The majority of counties fall in the $17.00–$20.00 per hour range.
- 283 hours per month * $18.66 = $5,281.58 per month
- 11% cases = $5,527,444,785.76 per year ($5.5 Billion)
Parents are encouraged to quit their jobs and “Get Paid To Stay Home With My Autistic Loved One”. Protective Supervision under California’s In-Home Supportive Services (IHSS) program provides 24-hour, non-medical supervision for individuals “who are at risk of injury when left alone”. Up to 195 hours per month are generally authorized for protective supervision for non-severely impaired autistic recipients; those with “severely impaired” status may be eligible for as many as 283 hours per month. At current IHSS wage rates, maximum authorized hours (195–283/month) translate to a significant monthly stipend for caregivers (often parents of autistic children) who provide qualifying supervision. WPCS (Waiver Personal Care Services) expenditures in California are a subset of IHSS spending, covering personal care hours and services for Medi-Cal recipients on the Home and Community-Based Alternatives (HCBA) Waiver.
California does not routinely publish IHSS protective supervision recipient data specifically filtered by “autism” diagnosis in public data dashboards. Most source data combine all cognitive or mental impairments. Older program analyses found that ~11% of IHSS recipients received protective supervision, mostly for cognitive or behavioral disabilities. Historically, recipients with cognitive or behavioral disabilities—including autism—make up about 20–25% of the IHSS caseload. Cognitive or behavioral disabilities are among the costliest IHSS categories due to the need for protective supervision and constant personal care.
SSI – Unemployable
SSI: number of SSI recipients 99,015 ($728.77 average payment = $73 million)
At most, 10% of autistic adults, or 1-2% of CDC prevalence ($730,000 cost).
SSI adult diagnostic tables typically report autistic disorders and “developmental disorders” together, possibly around 1%–3% for adults, though exact numbers for California are not published. A calculation using the CDC prevalence of SSI recipients yields no more than 3,194.68 (0.329%) Autistics on SSI. Thus, 99% of Autistics are employable and educable unless proven otherwise.
Leave a comment